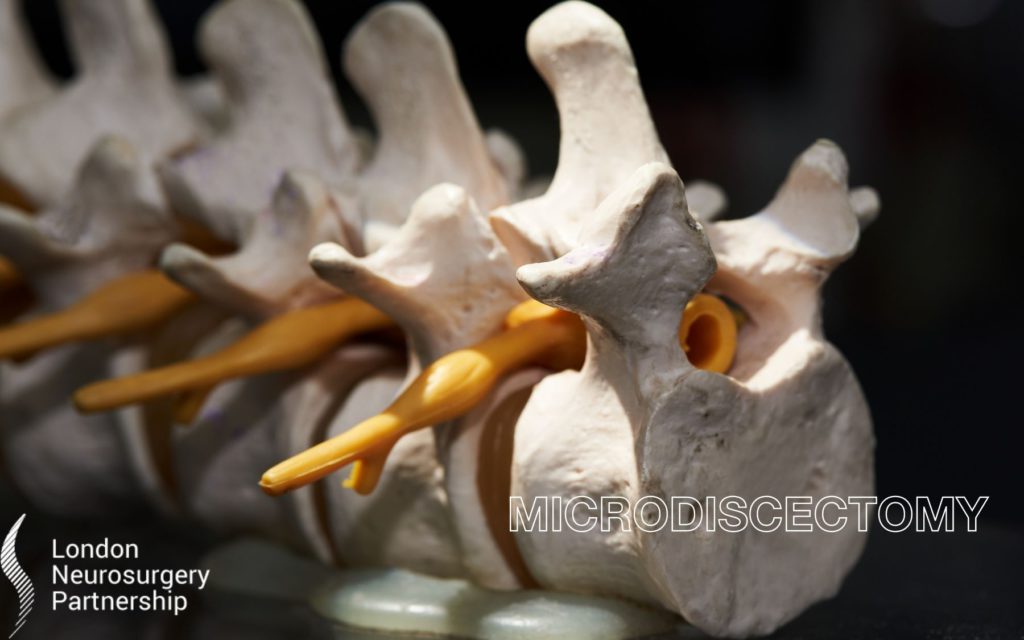
Mr Nicholas Thomas explains the procedure for a microdiscectomy.
A microdiscectomy is a minimally invasive surgical procedure used to treat patients who are suffering with a herniated lumbar disc. The aim of the surgery is to remove parts of the herniated disc from the lower back and alleviate their pain. It is a type of keyhole surgery and thanks to pioneering medical equipment and technologies we are able to perform such a procedure this way.
What is a herniated disc?
A herniated disc is when the soft tissue that sits between the individual bones of the spine pushes out through the spinal canal through a tear or rupture in the annulus.
What symptoms require a microdiscectomy for a herniated disc?
- Worsening sciatic pain
- No improvement using treatments
- Worsening muscle weakness and numbness
- If a patient got a herniated disc after a serious accident
Depending on the patient’s symptoms and how serious the herniated disc is will decipher on whether the patient does need to go ahead with surgery. Other simpler and less invasive treatments can be recommended before surgery is decided as many do work and mostly surgery is not necessary. Remember – surgery is always a last resort.
What risks of having a microdiscectomy are involved?
As with every procedure, risks are involved but with microdiscectomies complications are rare.
- Bleeding
- Nerve root damage
- Infection
- Recurrent disc herniation
- Bladder/bowel incontinence
- Blood clot
The surgery
A microdiscectomy is performed using general anaesthesia which means the patient will be fully unconscious during the operation. As stated above, the aim of the surgery is to improve the patient’s pain by removing the disc material that is putting pressure on the spinal cord.
A patient would have had MRI scans to discover and keep track of the herniated disc. Before surgery has taken place and new scan will be necessary to identify the area needed to operated and check for any changes.
The patient is positioned prone on the operating table. A microscope is used to enhance visualisation and see the affected area through a small tube clearly. X-ray is performed to locate the herniated disc and an incision is made to the skin. Retractors placed and fixated. X-ray and microscope used to visualise the spine. A burr is used to enter the spine and utilising microsurgical instruments, part of the ligamentum flavum is removed. The nerve root is gently mobilised using a ball tip probe and the nerve root is freed up and mobilised and retracted out of the way. Rongeurs are used to remove the herniated disc fragment. Retractors are removed and incision is closed with sutures.
Usually the patient will stay in hospital overnight and be discharged the following day. It takes a patient about 6 weeks to recover and during this time they will need to keep mobile without doing any heavy lifting or strenuous tasks. A follow up and scan with the surgeon will be necessary during a post-operative follow up to check all is ok.
This article is intended to inform and give insight but not treat, diagnose or replace the advice of a doctor. Always seek medical advice with any questions regarding a medical condition.


0 Comments